‘Less learning, more work’: PG medical students are struggling with NMC’s district residency programme
Sheena Sachdeva | July 7, 2023 | 12:40 PM IST | 5 mins read
National Medical Commission’s District Residency Programme has been introduced without adequate planning or preparation, complained PG students.
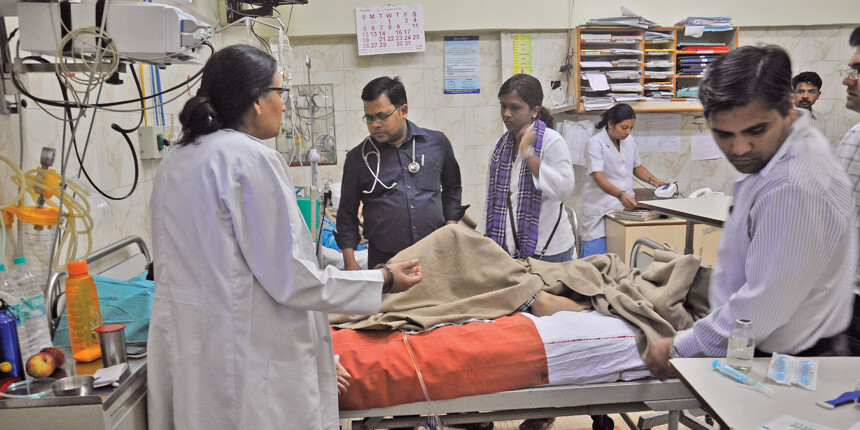
NEW DELHI: Rahul Kumar, a second-year postgraduate resident at Osmania General Hospital Hyderabad, has to travel 50 km every day to Area Hospital Patancheru, on the city’s periphery. He has been going since May to fulfil requirements of the District Residency Programme. Introduced by the National Medical Commission (NMC) in 2020, the DRP is a training programme for postgraduate students that simultaneously aims to address staffing shortages in district hospitals.
However, its hasty implementation on the heels of the Covid pandemic has caused widespread disruption. While all states started placing students from April and May, many did not hold up their end of the deal which was providing places to stay, paying for the commute and similar support. The students discovered they would be assigned district postings only in March.
“The revised notice of DRP mentions accommodation within the posted hospitals, and if the authorities cannot arrange it in the hospital, they should provide it in nearby places within 2-3 km. Further, transport facilities or charges will be provided along with proper safety for the resident doctors. But ironically, none of these are provided,” explained Kumar (name changed on request).
Resident doctors and their representative bodies across states like Maharashtra, Andhra Pradesh, Telangana, Madhya Pradesh and others, said that without proper planning, implementation of the DRP has been chaotic.
Also Read | Battling NEET coaching and boredom: Why AIIMS Delhi is changing the way it teaches
NMC rules
In December 2022 and January this year, the NMC issued notices making the three-month DRP mandatory for postgraduate medical students. NMC had earlier halted DRP’s implementation due to the Covid pandemic, resuming it from this year. The programme requires postgraduate medical students – residents – to spend three months serving at a district hospital. Postgraduate students of medicine are an important part of the healthcare workforce and hospitals away from major cities are usually short-staffed, explained Aviral Mathur, president, Federation of Resident Doctors Association (FORDA).
The DRP was made mandatory for the award of degree for all students admitted since 2021.
Telangana’s state resident doctors had boycotted work for 10 days in protest against lack of facilities provided for DRP in March this year; despite that, the state offered no support. “Because NMC has made the programme mandatory for all the resident doctors, and if we don’t work under DRP, we won’t get our degree, so we had to get back to our hospitals,” said Kumar.
Also Read | NExT exam will help students ‘focus on practical training’: MAMC head of medical education
Poor planning
All states started posting doctors around April and May but students were informed only in March, said Kumar. “Receiving a letter on March 21 was a shock. We would be placed somewhere else within a week with no clarity on travel or accommodation,” stated Kumar.
The postings also made workload distribution a problem in the city hospitals. With 30-35 percent of students posted in district and peripheral hospitals, those in city hospitals found their work increasing.
“NMC didn’t notice that due to Covid-19, most exams were postponed, which led to delays in starting new batches. So now, in most colleges currently, there are hardly any third-year residents available because either they are preparing for their exams or have graduated. Hence, all the workload is on first and second-year residents, and DRP has added to the chaos,” said Vardhman S Rothe, president, Nair Hospital and BMC, Maharashtra Association of Resident Doctors (MARD).
Also Read | District Residency Programme mandatory for all private medical colleges, deemed universities students: NMC
No facilities
Nikhil B Teja, joint secretary, Osmania Telangana Junior Doctors Association, Hyderabad, highlighted that most doctors travel 50-100 km daily without extra stipend or accommodation. “It’s difficult for doctors to travel three-four hours to the remote parts. No rooms or accommodations are available in the peripheral or district hospitals,” said Teja.
Sanjana Gupta (name changed), a second-year resident at Nair Hospital, Mumbai, added that doctors have been placed also in areas with Naxalite activity but with no security.
Even healthcare infrastructure is missing and residents specialising in particular fields are not getting trained in those fields. “Many resident doctors studying Doctor of Medicine (MD) or Master of Surgery (MS) are posted in the district hospitals where they are treating cough and cold cases, “said Gupta. “A postgraduate resident specialising in orthopaedics is treating patients at primary healthcare centres with minimal resources. “There are no instruments or equipment for basic tests like blood culture, CT-Scan or X-Ray and others. How will we treat the patients or even follow up with them?”
In some places, even proper food or canteens are not available, said Teja.
“After completing MBBS, people seeking a specialised career opt for masters or postgraduate studies. But it is ironic that residents are being trained in the opposite under DRP,” he explained.
District Hospitals: Less learning, more work
Doctors complain that because of poor planning, they are missing out on vital exposure in their chosen specialisations and are also behind in writing their thesis.
“During the residency, doctors must write a thesis. But due to the programme we are posted in different hospitals and lagging in our course work,” added Gupta. At the same time, work pressure is intense.
Many district hospitals have only a few consultants who come for brief periods and leave, placing the bulk of the workload on the residents. “In Maharashtra, residents are working both at their parent hospitals and district hospitals, leading to overload of work, even during leave. It’s like doing two jobs at once with no extra stipend or travel allowance,” said Rothe.
MARD took the issue to the Directorate of Medical Education and Research, Maharashtra, the state body overseeing medical education, but has yet to receive any relief.
Possible solutions
Most residents favour a policy that gives students more choice. “States like Andhra Pradesh allow residents to opt for district hospitals in their home cities,” said M Karuna Prasantha, second-year resident, department of community medicine, Andhra Medical College, Visakhapatnam, and president of Andhra Pradesh Junior Doctors Association. “Also, states should improve the facilities available at the district or peripheral hospital wherever residents are posted under DRP.”
In Madhya Pradesh, the state government is providing Rs 3,000-Rs 6,000 per month as a stipend based on city and district posting. But still, lack of infrastructure is a major problem, stated Swastik Bhardwaj, member, Resident Doctors Association, Madhya Pradesh.
Rothe approved of the DRP in general, finding the implementation and timing to be the problems. “The government should still incentivise residents to join the programme which can happen only through proper infrastructure and facilities,” said Bhardwaj adding that programme is ideal for third-year students, not first or second-year ones who are still learning.
“Currently, it’s a break in learning, but with inter-state posting or infrastructure and facilities, there are high chances residents will get attracted,” said Bhardwaj.
Follow us for the latest education news on colleges and universities, admission, courses, exams, research, education policies, study abroad and more..
To get in touch, write to us at news@careers360.com.